AI-Driven Dental Insurance Verification
RevenueWell's AI-driven insurance verification system fully replaces manual insurance verification with intelligent AI agents doing the work for you – more precisely and accurately. They confirm coverage, validate details, and deliver a clear, reliable report before every appointment. That means fewer admin tasks, fewer mistakes, and total confidence in every cost estimate you present to patients.


Proactive Appointment Prep Done for You
Automatic Coverage Verification
AI agents automatically verify patients’ coverage prior to their appointments. They access payer portals and cross-reference eligibility and benefits so you’re not scrambling to do it at the last minute.
Automatic Retry for Failed Verifications
They automatically retry any failed verifications, so no more portal hopping, long holds, or last-minute rechecks.
Dynamic Benefits Report
You receive a clean, easy-to-read report that includes a full explanation of benefits, past services, and eligibility dates for the procedure codes. The form automatically syncs to your PMS.
Patient Cost Estimates
You can use this information to provide patients with accurate cost estimates, improving trust and reducing unexpected balances.
Faster Verifications in Minutes. Accurate Information Every Time.
Skip the MFA Headaches
Multi-factor authentication (MFA) for payer portals can slow everything down. Instead of chasing verification codes or getting kicked out of portals, let the AI agents handle authentication for you. Our system manages MFA in the background, eliminating the need to remember and constantly re-enter your password. You keep working without interruptions.
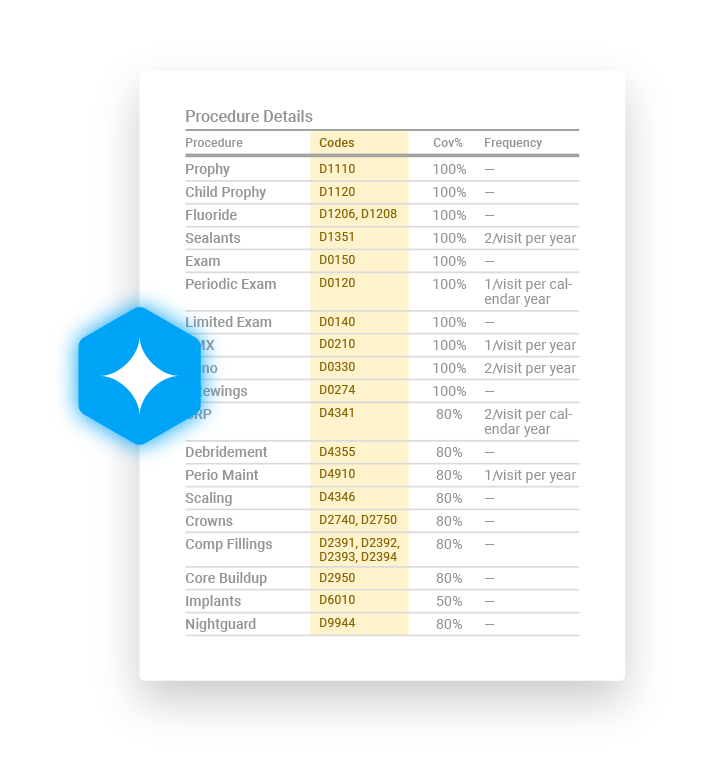
Insurance Reports You Can Easily Read
AI will send you an easy-to-understand report that includes an explanation of benefits, past services, and eligibility dates for the procedure codes. Each code displays whether the patient is eligible for a treatment now or when they will be. Clear reports reduce manual work and errors, helping your team have transparent cost conversations with patients and planning appointments accurately.

Pinpoint Procedure Codes
Insurance verification can support 800+ dental codes, ensuring your team can put together precise cost estimates. Less claim denials, better cash flow your practice.
Catch Coverage Issues Early
When a patient schedules an appointment or shares their insurance details, AI performs the verification for you. Get clued into potential issues early, so you can double-check insurance in advance. No more check-in surprises.
A System You Can Rely On

Shrink Your Workload
AI agents take care of verifying insurance for you. You avoid time-consuming calls, portal hopping, and rework, freeing you up to spend time with patients.

Speed Without Cutting Corners
AI completes insurance verifications in minutes, not hours or days, while still reviewing the same details your team looks for, just faster and more consistently. With AI, up to 80% of your appointments can be handled each day.

Strengthen Every Patient Relationship
By automating the verification process, practices provide transparency, earn patients’ trust, and keep them coming back (and referring others).

More Predictable Revenue
When coverage and estimates are correct from the start, collections improve and write-offs decrease.

Fewer Claim Denials
Cleaner, more accurate verifications upfront mean fewer surprises, and fewer claims kicked back for missing or incorrect information.

Increased Case Acceptance
Patients are more likely to move forward with treatment when they clearly understand what insurance covers and what their portion will be. Accurate, upfront estimates help eliminate hesitation and support higher case acceptance.

From Insurance to Revenue Without the Guesswork
Insurance verification isn’t a siloed process at your practice. It’s the starting point of clean claims and when it’s automated, the rest of your revenue cycle runs smoother. Revenue Cycle Management connects verification and claims tasks together with AI-driven automation, helping practices reduce errors and denials, and create more consistent cash flow.
One Less Bottleneck, One Stronger System
Insurance verification shouldn't slow your practice down. See how AI-driven automation helps your team do less manual insurance work, prepare earlier, and keep revenue moving.

